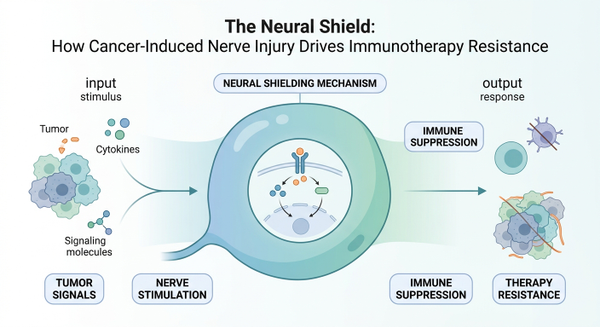
The Neural Shield: How Cancer-Induced Nerve Injury Drives Immunotherapy Resistance
For years, our understanding of cancer focused primarily on the tumor cells themselves and the immune system's response. However, a groundbreaking wave of research is revealing a startling truth: nerves, long considered mere conduits for pain or sensation, are actively co-opted by cancer to build a formidable 'neural shield,' driving resistance to even our most advanced immunotherapies. This paradigm shift is reshaping how we view the battle against cancer.
Introduction
Immunotherapy has revolutionized cancer treatment, offering unprecedented hope for many patients by harnessing the body's own immune system to fight malignant cells. Yet, a significant challenge remains: a substantial portion of patients either do not respond to these therapies or develop resistance over time. This resistance is often attributed to the complex and immunosuppressive tumor microenvironment. Recent discoveries, however, are pointing to an unexpected culprit: the intricate interplay between the nervous system and cancer, collectively known as the neuro-immune axis. Understanding these neuro-immune interactions is now recognized as offering novel therapeutic cancer targets, paving the way for new strategies to overcome immunotherapy failure.
The Unseen Sabotage: How Cancer Corrupts Nerves to Evade Immunity
The concept of cancer-induced nerve injury (CINI) has emerged as a critical mechanism underlying immunotherapy resistance. Far from being passive bystanders, nerves within and around tumors are actively damaged by cancer cells. A pivotal 2025 study published in Nature unveiled that cancer cells directly degrade the protective myelin sheaths surrounding nerve fibers. This nerve injury doesn't just happen; it triggers a cascade of events, initiating a chronic inflammatory response. This inflammation, in turn, creates an immunosuppressive environment that effectively shields tumors from the immune system's attack, particularly hindering the efficacy of anti-PD-1 therapies. Essentially, nerve injury triggers chronic inflammation shielding tumors, turning what should be an immune-activating response into a barrier against treatment.
Beyond Injury: Tumors' Masterful Manipulation of Neuroimmune Circuits
The influence of the nervous system extends beyond direct injury. Research indicates that tumors are adept at hijacking entire neuroimmune circuits to facilitate their escape from immune surveillance. This involves a complex interplay where cancer cells manipulate neural signals and pathways to their advantage. For instance, studies have shown that tumors hijack neuroimmune circuits for immune evasion, orchestrating a sophisticated defense mechanism. This manipulation can involve various components of the nervous system, including sensory neurons, which are increasingly recognized as pivotal players in both cancer progression and the associated pain. The multifaceted role of these neurons highlights the depth of cancer's neural infiltration.
Neurotransmitters: Unmasking the Molecular Messengers of Resistance
Delving deeper into the molecular mechanisms, scientists are uncovering how specific neurotransmitters act as key players in driving immunotherapy resistance. These chemical messengers, traditionally associated with brain function, are now known to be secreted by both nerve cells and cancer cells within the tumor microenvironment. Their presence can significantly alter the immune landscape, creating conditions unfavorable for immune cell activity. A 2025 study in Molecular Cancer highlighted that neurotransmitters drive resistance to immune checkpoint inhibitors. This suggests that targeting these specific neurotransmitter pathways could offer a novel approach to disarm the neural shield and enhance the effectiveness of existing immunotherapies. It's a testament to the intricate molecular dialogue occurring between cancer and the nervous system.
The Glioma Connection: Neuron-Glioma Interactions and Immunosuppression
While the broader concept of cancer-induced nerve injury applies across various tumor types, specific contexts like gliomas offer unique insights into neuro-immune interactions. In diffuse midline gliomas, for example, the complex relationship between neurons and glioma cells actively modulates the tumor immune microenvironment. This interaction contributes to the immunosuppressive nature of these aggressive brain tumors, making them particularly challenging to treat with immunotherapy. Research into these specific neuron-glioma interactions modulating the tumor immune microenvironment is crucial. Understanding how these cellular dialogues foster immune evasion in the brain can inform targeted strategies to break down the neural shield in these difficult-to-treat cancers, potentially unlocking new therapeutic avenues for patients.
Dismantling the Neural Shield: A New Frontier in Cancer Therapy
The revelation that cancer actively exploits the nervous system to create a 'neural shield' against immunotherapy marks a significant turning point in oncology. From direct nerve injury and chronic inflammation to the sophisticated manipulation of neuroimmune circuits and neurotransmitter signaling, the nervous system is no longer a passive bystander but an active participant in tumor progression and immune evasion. By understanding these intricate mechanisms, researchers are now poised to develop innovative strategies to dismantle this neural shield. Targeting cancer-induced nerve injury, modulating specific neurotransmitter pathways, or disrupting neuron-glioma interactions could unlock new therapeutic opportunities, ultimately improving patient responses to immunotherapy and offering renewed hope in the fight against cancer.
References
- Baruch EN, Gleber-Netto FO, et al. (2025). Cancer-induced nerve injury promotes resistance to anti-PD-1 therapy. Nature. 646(8084):462-473. PMID: 40836096
- Zhang Y, Guo Y, et al. (2025). Cancer cells co-opt an inter-organ neuroimmune circuit to escape immune surveillance. Cell. 188(24):6754-6773.e29. PMID: 41138728
- Zhang C, Guo X, et al. (2025). The neuro-immune axis in cancer: from mechanisms to therapeutic opportunities. J Hematol Oncol. 18(1):93. PMID: 41152924
- Yang J, Wu Y, et al. (2025). Neurotransmitters: an emerging target for therapeutic resistance to tumor immune checkpoint inhibitors. Mol Cancer. 24(1):216. PMID: 40790592
- Davis BM, McIlvried LA, et al. (2025). Rethinking relief: Targeting sensory neurons to combat cancer and pain. Cancer Cell. 43(10):1777-1782. PMID: 40780214
- Liu J, Ha JH, et al. (2025). Adaptive immunotherapeutic paradigms in diffuse midline glioma: integrating epigenetic reprogramming, neuron-glioma interactions, and tumor microenvironment modulation. J Neurooncol. 176(2):144. PMID: 41460355
Recent Posts
-
The Neural Shield: How Cancer-Induced Nerve Injury Drives Immunotherapy Resistance
For years, our understanding of cancer focused primarily on the tumor cells themselves and the immu …29th Mar 2026 -
Metabolic Bloodhounds: Engineering Immune Cells to Track Cancer's Chemical Trail
Imagine a specialized squad of immune cells, meticulously trained and equipped, not just to fight c …27th Mar 2026 -
Mitochondrial Transplantation: A New Frontier in Restoring Neural Function After Ischemic Stroke
Imagine a future where the devastating impact of a stroke could be significantly mitigated, not jus …27th Mar 2026